Evaluating a cholesterol screening: Risk appraisals, outcome expectancies, and self-efficacy beliefs as predictors of physical exercise and alcohol consumption
André Hahn *
Institute of Educational Psychology, Humboldt-University of Berlin
and
Thomas von Lengerke
Sport Science III, Technical University of Chemnitz
[This document in Portable Document Format (PDF) by Adobe. For viewing and printing Acrobat Reader 3.0 is necessary.]
One major objective of the "Berlin Risk Appraisal & Health Motivation Study" (BRAHMS) has been to examine the impact of individualized feedback about personal risk factor status on health behavior. 1518 adults participated in a public blood cholesterol screening. The test result was explained to each participant individually in terms of its meaning and potential impact on his or her health. Several health cognitions and behaviors were assessed using specific questionnaires, and compared to those of a control sample (N=639). 619 of the screening group (40%) and 436 of the controls (68%) completed a follow-up questionnaire six months later. The present analysis focuses on changes in two health behavior domains, physical exercise and alcohol consumption. Three factors specified by social-cognitive health behavior theories were considered as possible predictors: (1) Risk appraisals, defined as the product of the estimated probability of getting cholesterol-related diseases, and their perceived severity; (2) behavior-specific outcome expectancies, distinguishing between expected benefits and expected costs; and (3) self-efficacy beliefs as factors fostering health behaviors particularly when one encounters obstacles and barriers to change. Overall, the results are in line with expectations. First, screening participation itself, i.e., regardless of the test result, influenced the amount of physical exercise and alcohol consumption in a health-promotive fashion. Second, screening participants with a pathological level of cholesterol estimated their health risk to be much higher than that of those with more favorable levels and control subjects. High risk appraisals resulted in a remarkable reduction of the alcohol consumed, whereas no impact was observed in terms of an increase in physical exercise. Third, outcome expectancies - particularly benefits - and self-efficacy beliefs were predictive of self-reported changes in behavior. However, the joint function "risk appraisal x outcome expectancies x self-efficacy", despite its theoretical significance, failed to account for additional variance in the behavioral measures. The results are discussed in terms of their implications for improving risk factor screenings as measures of behavior-oriented prevention. Specifically, it is concluded that outcome expectancies and self-efficacy beliefs should be strengthened especially in individuals with pathological test results, but cognitions detrimental to health-promotive behavior.
KEY WORDS: Screening, cholesterol, physical exercise, alcohol consumption, health cognitions, risk appraisals, self-efficacy, outcome-expectancies
Introduction
Screening for prevention is concerned with actively seeking to identify a disease or pre-disease condition in people who are presumably healthy (Orbell & Sheeran, 1993). The impact of screenings like a cholesterol test, as the one we conducted in our study, depends on a number of factors. Here, recent reviews like Theresa Morteau’s 1993 paper critize that most studies are only descriptive in nature, focusing exclusively on behavioral and physiological consequences of screenings, but neglecting variables which are likely to moderate or mediate the effects of a screening programme. This may ultimately result in an underestimation of the importance of health screenings. One of the most prominent mediating factors proposed in the literature are personal risk appraisals following the communication of the test result. Most health psychologists assume that the motivational process to alter one’s current health-behavior starts with the belief that one faces a substantial risk of experiencing harm. In our context: If I had not planned to change my behavior before the screening, why else, if not because of - now known - high risk, should I do so afterwards?
Table 1 Risk perceptions in health behavior theories
| Abreviation | Theory | Authors |
| HBM | Health Belief Model | Becker, 1974; Rosenstock, 1990 |
| PMT | Protection Motiviation Theory | Rogers, 1983 |
| SEU | Subjective Expected Utility Theory | Edwards, 1961; Sutton, 1982 |
| TRA | Theory of Reasoned Action | Fishbein & Ajzen, 1975 |
| TSB | Theory of Social Behavior | Triandis, 1980 |
| TPB | Theory of Planned Behavior | Ajzen, 1991 |
| TT | Theory of Trying | Bagozzi, 1992 |
| PAP | Model of the Precaution Adoption Process | Weinstein, 1988 |
| HAPA | Health Action Process Approach | Schwarzer, 1996 |
Risk appraisal - more commonly labeled "perception of personal susceptibility" - is a central variable in most theories of self-protective behavior (for reviews, see Wallston, 1994; Weinstein, 1993; Schwarzer, 1996). The classic Health Belief Model, the Protection Motivation Theory, or the Health Action Process Aproach are examples (Table 1). But all of these models assume that the appraisal of a high risk is only but one out of a number of necessary components in the process of behavioral change. From our point of view, when we try to reduce the number of these other proposed factors to their core concepts, only two general factors remain. These are best represented by labels used by Albert Banduras (1977, 1986, 1997) in his Social Cognitive Theory: Outcome and self-efficacy expectancies.
Table 2 Outcome expectancies and self-efficacy expectancies in other health behavior theories
Outcome expectancies |
Self-efficacy expectancies |
| Cognitions of the type: Action/Non-Action è Outcomes |
Cognitions of the type: Person è Action |
|
|
On one hand, outcome expectancies refer to the expected positive and negative consequences of both acting and not acting. Thus, they are equivalent to concepts like normative and personal behavioral beliefs, perceived costs and barriers, reponse efficacy, or precaution effectiveness (Table 2). Self-efficacy, on the other hand, refers to the perceived own capablilities to perform courses of action required to attain the desired outcomes. The term self-efficacy is consistently used by most theorists. There are a few models originally not including self-efficacy, but reinterpretated existing concepts like "barriers" as being very similar to self-efficacy beliefs. Still others used slightly different labels, for instance "perceived behavioral control", but acknowledged the similarity with self-efficacy (Table 2).
In sum, we assume that the likelihood with which people will adopt a valued health behavior (such as physical exercise) or give up a detrimental habit (such as alcohol consumption) depend on only three sets of cognitions:

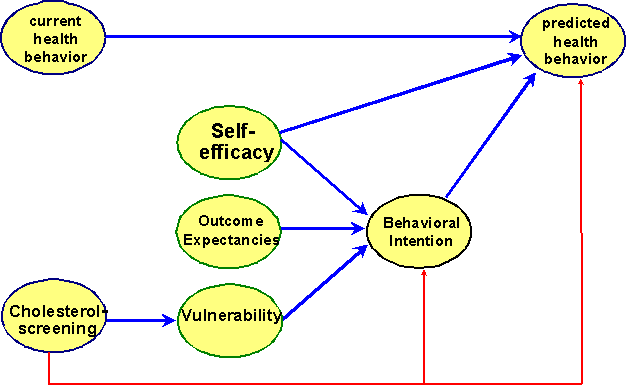
Figure 1 Theoretical framework of the cholesterol screening programme
The present study explores these propositions in predicting both intention formation and health behavior change in the context of a public cholesterol screening program (Figure 1). All three factors mentioned should clearly increase the amount of explained variance in intentions and health behaviors when compared to the effect of the cholesterol screening alone. The screening itself and the communication of the test results are regarded as the triggering stimuli for re-appraising one’s own health risk or vulnerability. Methodologically speaking, we assume vulnerability to be a mediator variable of the cholesterol screening on intentions and health behavior. Furthermore, the effect of the mediator "vulnerability" could be moderated both by outcome expectancies and self-efficacy. This hypothesis is based on similar ideas within Roger’s Protection Motivation Theory, which assumes high values on all three factors to be a necessary condition for intention formation. This multiplicative combinational rule implies triple interactions between vulnerability, outcome expectancies, and self-efficacy.
Method
Subjects, Design and Procedure
Participants of the cholesterol screening group were 1 518 residents of Berlin at four different locations (two Universities and two city halls). Fourty-seven percent of the voluntary participants were male, and they were, on average, 41 years old. On arrival at the study site, participants received a questionaire, which included a portion of the relevant measures used for data analysis. Afterwards, a cholesterol test was taken and participants were immediately provided with their test results. Each participant was informed whether his or her result indicated a normal, a borderline, or a high cholesterol level. 817 persons or 54% of the first wave sample completed a follow up questionaire six months later. The high attrition rate is due to the extraordinary expenditure necessary to take part at the second cholesterol screening, and responding to about 500 items again. The responses of the screening group were compared to those of a control sample consisting of 639 people. Of the control group 436 (68 %) completed a follow-up questionnaire half a year later.
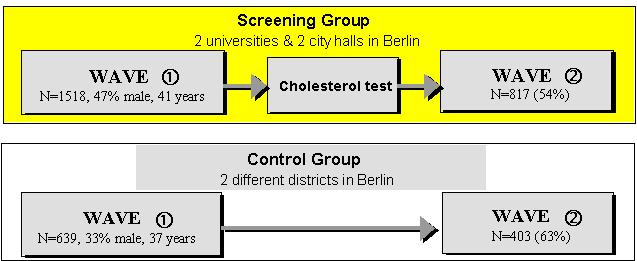
Figure 2 Study design and sample characterstics
Instruments
In order to assess the constructs mentioned above, we had to develop items and scales that, while being new, also rely on published material to a high extent (see Table 3). Vulnerability was assessed by multiplying two reliable scales measuring the perceived susceptibility and severity of five cholesterol-related diseases. Outcome expectancies with regard to the reduction of alcohol consumption and engaging in physical activity were measured by short scales asking for expected positive and negative consequences separately. An example is: "If I would drink less alcohol, then that would mean a loss of quality of life for me." In order to simplify the subsequent analyses, positive and negative outcome expectancies, which do not correlate with each other, were combined to a ratio score: benefits minus costs. Perceived self-efficacy for physical exercise was measured by 9 four-point items such as "I would be able to do a planned sports activity even if the weather is bad". Perceived self-efficacy to reduce the amount of alcohol consumption were measured by three items with a satisfying internal consistency of .79. Behavioral intentions were measured by single items with a 7-point response format. The questionnaire extensively assessed the participants’ health behavior. Physical exercise consisted of the frequency of various types of activities, and the time spend on those activities. Alcohol consumption was assessed to take into account the frequency and the quantity of drinking as well as the amount of alcohol within four different types of drinks. For these variables, indices were calculated representing the amount of pure alcohol consumed per week, and the frequency of sports activities per week.
Table 3 Measurement of the study variables: Vulnerability, outcome expectancies, self-efficacy expectancies, behavioral intentions and health behavior
| Vulnerability |
Susceptibility (5 items, alpha=.85) |
Severity (5 items, alpha=.86) |
| Outcome expectancies |
Sports and Physical Activity (positive expectancies, 5 items,
alpha=.72, negative expecanties, 5 items, alpha=.85) |
Alcohol (positive expectancies, 5 items, alpha=.85, negative
expecanties, 2 items, alpha=.78) |
| Self-efficacy |
Sports and Physical Activity (9 items, alpha=.94) |
Alcohol (3 items, alpha=.79) |
| Intentions |
Sports: "I intend to do sports activities regularly (at least once a week) during the next months. [1] I do not at all have this intention – [7] I definitely have this intention" |
Alcohol: "I intend to drink less alcohol during the next months. [1] I do not at all have this intention – [7] I definitely have this intention" |
| Behavior |
Sports: "How often do you usually do the following sports activities?": (1) Cycling, (2) Exercises, Gymnastics, Aerobics, Dancing, (3) Stamina sports, (4) Strength events, (5) Martial arts, (6) Playing sports, (7) Hiking, Walking - [1] (almost) daily, [2] several times a week, [3] once a week, [4] 1-3 times a month, [5] seldom or never |
Alcohol: "How often do you drink the following
alcoholic beverages? On occasions when you drink alcoholic beverages, how much do you
drink?: (1) beer, (2) wine, sparkling wine, fruit wine, (3) Cocktails, Liqueurs, Vermouth,
(4) High-proof alcoholic beverages (Rum, Brandy, Schnapps) |
Results
When carrying out a health screening, the first question an employer would ask his agent is whether there were any direct effects. One desired outcome would be a change in health behavior in response to the screening. As depicted in figure 3 and figure 4, this was not fulfilled by our intervention.
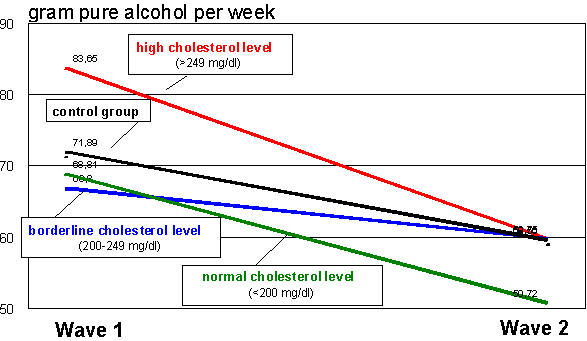
Figure 3 Behavioral change: alcohol consumption
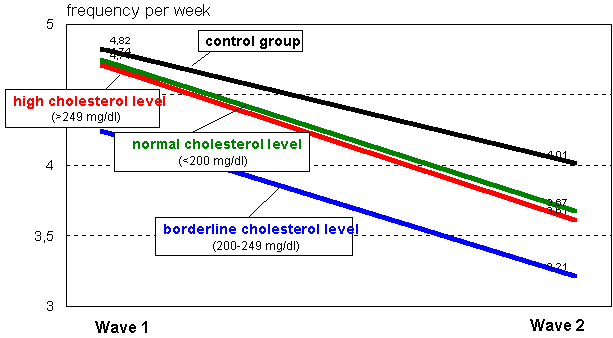
Figure 4 Behavioral change: physical exercise
There was a general decrease in alcohol consumption over time for all four groups of interest (F(1,1365) = 51,1, p < .001). There seems to be a higher decrease in the high risk group with cholesterol levels above 250 units. But the repeated measurement analysis of variance didn’t show a significant time by group interaction (F(3,1365) = 1,75, p = .15). Thus, neither is there a simple screening effect, nor is there, when comparing the three risk groups, a direct risk-communication effect (F(1,1365) = 1,37, p = .25).
The same hold even more with regard to changes in physical activity. Again, there is a decrease over time, which could be interpreted as seasonal effect, because the second wave took place at the end of the year (F(1,1388) = 127,7, p < .001). But again, this decrease is not differential (Interactionterm, F(3,1388) = 0,64, p = .59).
When there are no direct main effects, it is possible that the variables proposed by health psychologists can alter these negative results by clarifying the conditions under which screening effects can be observed. Consequently, we looked at the most proximal effect variable studied, the scores on perceived vulnerability (Figure 5).
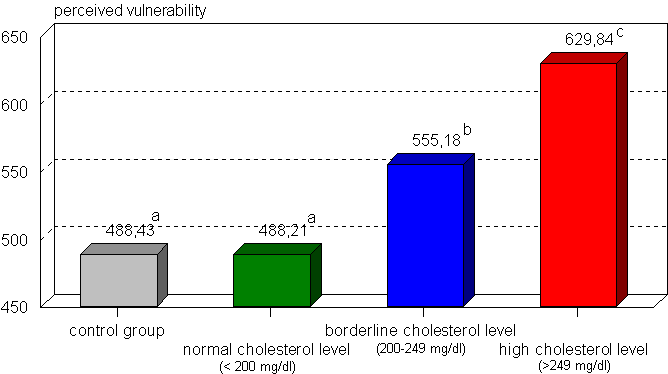
Figure 5 Comparing levels of perceived vulnerability: Control group, and three different screening groups
As hypothesized, there is a clear risk communication effect (F(3,1705) = 40,26, p < .001). The risk appraisals are in line with the communicated test results. Because the scores of the control group are comparable to the group with normal cholesterol levels, screening participants overall perceive themselves more vulnerable to the health risks under study.
If the perceived vulnerability could be successfully altered, immediately the question arises whether changes in health behavior depend on the vulnerability scores, and whether or not the hypothesized vulnerability-health behavior link is moderated by outcome expectancies and self-efficacy beliefs. Again, we first report the results for alcohol consumption as revealed by a four factor repeated measurement analysis of variance (Figure 6).
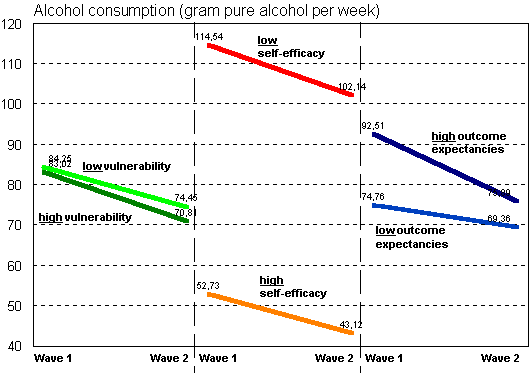
Figure 6 Changes in alcohol consumption as a function of perceived vulnerability, outcome expectancies and self-efficacy
Figure 6 depict changes in alcohol consumption over time separted for groups scoring low and high on vulnerability, self-efficacy, and outcome expectancies. It can be seen that there is no influence of vulnerability on the amount of weekly consumed alcohol. Groups scoring high and low on self-efficacy can be destinguished very clearly regarding their alcohol consumption (F (1, 631) = 71.7, p < .001). But the decrease over time equals for both efficacy groups. Therefore it cannot be stated that self-efficacy is a causal agent in health behavior change. However, there is a significant time by outcome expecanties interaction on alcohol consumption (F (1, 631) = 3.76, p = .05). That is, people expecting more benefits than costs in reducing alcohol consumption in fact had reduced their consumption six months later when compared to the group with unfavorable outcome expectancies. There were no further effects. Especially, there were no higher order interactions as proposed.
The result pattern for physical activity is very close to the results for alcohol consumption (Figure 7). First, there is again no direct influence of vulnerability on the altered frequency of physical activity. Although, the decline for people scoring high on the vulnerabity measure seem to be slightly smaller, this trend is not significant. Second, again participants scoring high on self-efficacy are better of regarding their behavior (F (1, 698) = 61.6, p < .001). But the general decline of physical activity equals in both groups. The same holds for outcome expectancies (F (1, 698) = 14.1, p < .001). Here the decrease in sports is independ of the expected utility of the behavior. Again, there were no further interaction effects.
In the last step of our analysis we tried to complete the picture by calculating two separate path analysis including all variables under study. In order to simplify the analysis, we used reliability corrected manifest variables instead of modelling latent constructs, which is much more lavish, and in most cases lead to comparable results. The analysis were done with LISREL 8 (Jöreskog & Sörbom, 1993).
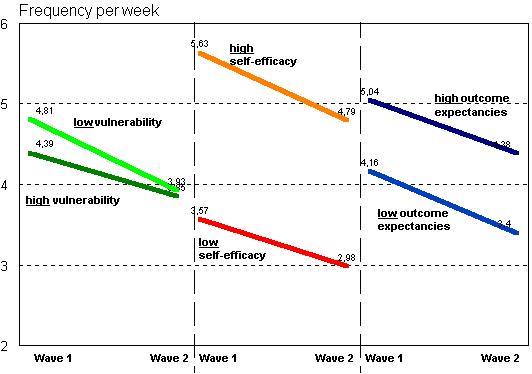
Figure 7 Changes in physical activity as a function of perceived vulnerability, outcome expectancies and self-efficacy
As can be seen in figure 8, the strongest direct path of our starting point, the cholesterol screening, is - as hypothesized - on the vulnerability. Thus, it can again be said that the risk appraisals are in accordance with the screening. Most interesting, a path of the screening goes to behavioral intention directly. This means, that there are features within the screening fostering intention formation which goes beyond the re-appraisal of one’s health risk. One of this unmeasured features might be new knowledge regarding the causes and impact of high cholesterol levels on health. There are two more factors influencing the intention to drink less alcohol in the future: outcome expectancies and the current amout of alcohol consumed. Participants with favorable expectancies and higher consumption levels intent to a higher degree to change their current behavior. So far the results are in line with our model proposed earlier. Unexpected is of course the missing link between self-efficacy and behavioral intention, as well as the missing link between intention and alcohol consumption at the second point of measurement. For the former one, we did not find any empirical reasons. It is just as it is. The missing power of intention to predict changes in alcohol consumption is at least partly due to the interindividual high stability of the behavior. About 65% of the variance at time 2 can be explained by the behavior six months earlier. This does not surprise too much considering earlier studies on the stability of health behaviors’ distributions.
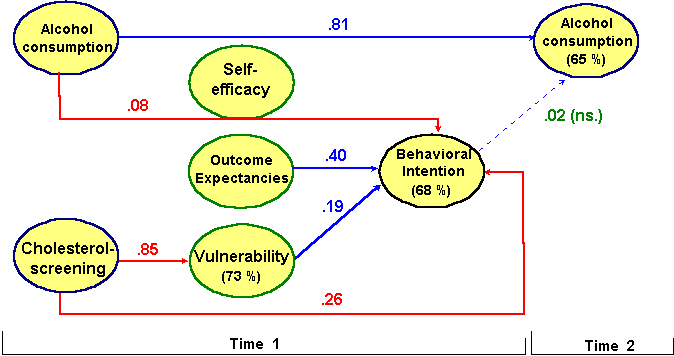
Figure 8 Predicting alcohol consumption: a path analysis (Note. insignificant paths and all intercorrelations are omitted. N= 621, Fit-Indices: Chi-Square(df=6) = 5.75 (p = 0.45), SRMR=0.01, GFI = 1.00, AGFI=0.99)
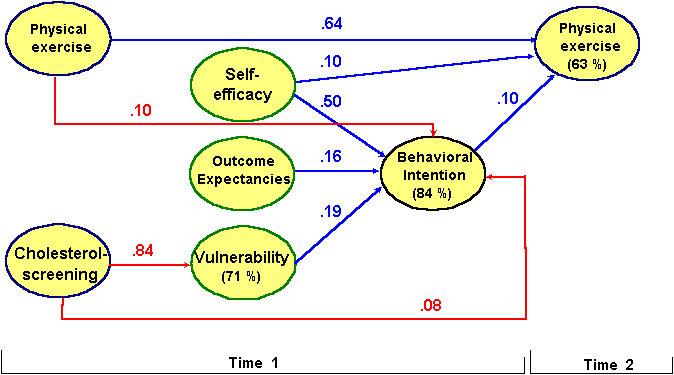
Figure 9 Predicting physical exercise: a path analysis (Note. insignificant paths and all intercorrelations are omitted. N= 698, Fit-Indices: Chi-Square(df=3) = 5.05 (p = 0.17), RMR= 0.05, SRMR=0.0073, GFI = 1.00, AGFI=0.98)
With reference to physical exercise the results are more in line with general expecations (Figure 9). In sum, the structur of the relationsships is very similar to the one just presented besides the resurrection of self-efficacy and behavioral intention. The intention to do sports activities regularly can be predicted by all five factors under study, and is mostly influenced by self-efficacy, followed by vulnerability and, outcome expectancies. Altogether, 84% of the intention’s variance are explained. Moving to the behavior at time 2, the behavior at time 1 has again the strongest direct influence. Of the cognitions, only self-efficacy and behavioral intention have the power to explain additional variance of the time 2 activity level. This is in line with the theory of planned behavior by Icek Ajzen (1991), and with the Health Action Process Aproach by Ralf Schwarzer (1996).
Discussion
Let us briefly summarize the results. One major goal of the study was to examine the effects of individualized information about a health risk on changes in various risk-related health behaviors. For this presentation we selected two health behavior domains, which are associated with cholesterol levels: physical exercise and alcohol consumption.
Overall, our results are only partial in line with common expectations. First, neither the screening itself, nor the individual test results of the screening participants influenced the amount of physical exercise and consumed alcohol per week in a positive way. Second, screening participants with pathological high levels of cholesterol estimated their health risk much higher than participants with more favorable cholesterol levels, and control subjects. Thus, the often quoted unrealistic optimism regarding health risks could be corrected by means of the screening program. Third, these higher risk appraisals were unrelated to changes in health behavior, but resulted in moderate higher behavioral intentions to alter the current behaviors. Fourth, the proposed influence of risk appraisals on changes in health behavior were neither moderated by outcome expecancies nor by self-efficacy beliefs. Therefore, we – as well as others before – failed to add empirical effidence to the theoretical important joint function "risk appraisal by outcome expectancies by self-efficacy". Fifth, personal expectancies regarding the consequences of behavioral change proved their importance on forming behavioral goals. Furthermore, analysis revealed, that favorable expectancies resulted in a reduction of the consumed alcohol. This result could not be replicated in the case of physical activity. Sixth, we found perceived self-efficacy to be closely associated with current health behavior. Surprisingly in the case of alcohol consumption, high self-efficacy beliefs were unrelated to both, intentions and changes in behavior. However, this negative result was somewhat corrected in the domain of physical activity. In line with studies by Godin, Valois, and Lepage (1993), and Fuchs (1996) we found perceived self-efficacy to be a (weak) predictor of physical activity. Seventh, the more causal quality of the four proposed moderator and mediator variables of the screening program in the process of health behavior change could hardly be established, because of the high stability of the health behavior under study.
If one thinks of optimizing cholesterol screenings, an important implication of our results would be to do more than just communicating the test results, and distribute some informative material. Interventions must concentrate more on activities that seem to be able to strengthen individual outcome expectancies and self-efficacy beliefs especially in those with pathological test results but behavior corrupting cognitions.
Acknowlegdements
This research was supported by the Deutsche Forschungsgemeinschaft (DFG; Internet: http://www.dfg-bonn.de/), and the Techniker Krankenkasse für Berlin und Brandenburg (TK: Internet: http://www.tk-online.de/). The authors wish to thank Britta Renner, and Ralf Schwarzer for their helpful comments on the first draft of this paper.
References
Ajzen, I. (1991). The theory of planned behavior. Organizational Behavior and Human Decision Processes, 50, 179-211.
Bagozzi, R.P. (1992). The self-regulation of attitudes, intentions, and behavior. Social Psychology Quarterly, 55, 178-204.
Bandura, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review, 84, 191-215.
Bandura, A. (1986). Social foundation of thought and action: A social cognitive theory. Engelwood Cliffs, NJ: Prentice-Hall.
Bandura, A. (1992). Self-efficacy and human functioning. In R. Schwarzer (Ed.), Self-efficacy. Thought control of action (pp. 3-38). New York: Hemisphere.
Bandura, A. (1997). Self-efficacy. The exercise of control. New York: Freeman.
Becker, M. H. (Ed.) (1974). The health belief model and personal health behavior. Thorofare, NJ: Slack.
Edwards, E. (1961). ‚Behavioral decision theory‘, Annual Review of Psychology, 12, 473-498.
Fishbein, M., & Ajzen, I. (1975). Belief, attitude, intention and behavior: An introduction to theory and research. Reading, MA: Addison-Wesley.
Fuchs, R. (1996). Causal models of physical exercise participation: Testing the predictive power of the construct "pressure to change". Journal of Applied Social Psychology, 26, 1931-1960.
Godin, G., Valois, P., & Lepage, L. (1993). The pattern of influence of perceived behavioral control upon exercising behavior: An application of Ajzen’s theory of planned behavior. Journal of Behavioral Medicine, 16, 81-102.
Jöreskog, K. & Sörbom, D. (1993). New features in LISREL 8. Chicago, IL: Scientific Software International.
Kirscht, J. P. (1988). The Health Belief Model and predictions of health actions. In D.S. Gochman (Ed.), Health Behavior (pp. 27-41). New York: Plenum.
Marteau, T. M. (1993). Health-related screening: Psychological Predictors of uptake and impact. In S. Maes, H. Leventhal, & M. Johnston (Eds.), International Review of Health Psychology (Vol. 2, pp. 29-49). New York: Wiley.
Norman, P., & Conner, M. (1996). The role of social cognition models in predicting health behaviours: Future directions. In M. Conner & P. Norman (Eds.), Predicting health behaviour: Research and practice with social cognition models (pp. 197-225). Buckingham: Open University Press.
Orbell, S. & Sheeran, P. (1993). Health psychololy and uptake of preventive health services: A review of 30 years’ research on cervical screening. Psychology and Health, 8, 417-433.
Rogers, R. W. (1983). Cognitive and physiological processes in fear appeals and attitude change: A revised theory of protection motivation. In J. R. Cacioppo & R. E. Petty (Eds.), Social psychophysiology: A sourcebook (pp. 153-176). New York, NY: Guilford Press.
Rosenstock, I. M. (1974). The Health Belief Model and preventive health behavior. Health Education Monographs, 2, 354-386.
Rosenstock, I. M. (1990). The Health Belief Model: Explaining health behavior through expectancies. In K. Glanz, F. M. Lewis & B. K. Rimer (Eds.), Health behavior and health education: Theory, research, and practice (pp. 39-62). San Francisco, CA: Jossey-Bass.
Schwarzer, R. (1994). Optimism, vulnerability, and self-beliefs as health-related cognitions: A systematic overview. Psychology and Health, 9, 161-180.
Schwarzer, R., & Fuchs, R. (1996). Self-efficacy and health behaviours. In M. Conner & P. Norman (Eds.), Predicting health behaviour: Research and practice with social cognition models (pp. 163-196). Buckingham: Open University Press.
Sutton, S. R. (1982). Fear-arousing communications: A critical examination of theory and research. In J. R. Eiser (Ed.), Social psychology and behavioral medicine (pp. 303-338). Chichester: Wiley.
Triandis, H.C. (1980). Values, attitudes, and interpersonal behavior. In M.M. Page (Ed.), Nebraska symposium on motivation. Lincoln: University of Nebraska Press.
Wallston, K. A. (1994). Theoretically based strategies for health behavior change. In M. P. O'Donnell & J. S. Harris (Eds.), Health promotion in the workplace (pp. 185-203). Albany, NY: Delmar.
Weinstein, N. D. (1988). The precaution adoption process. Health Psychology, 7, 355-396.
Weinstein, N. D. (1993). Testing four competing theories of health-protective behavior. Health Psychology, 12, 324-333.
Note. To whom correspondence should be addressed: André Hahn, Humboldt-University of Berlin, Institute of Educational Psychology, Geschwister-Scholl Str. 7, 10099 Berlin, Germany, phone +49-30-2093-4024, Fax +49-30-2093-4024, Email: hahn@psychologie.de, Web: http://www.psychologie.de/hahn/; Thomas von Lengerke, Technical University of Chemnitz, PHIL - Sport Science III, 09107 Chemnitz, Germany, phone +49 371 531-2939, fax-- +49 371 531-2935, Email tvl@phil.tu-chemnitz.de. This paper is based on a presentation held at the 11th Conference of the
European Health Psychology Society (Bordaux, September 3-5, 1997, France).© Copyright 1998 André Hahn & Thomas von Lengerke
[27. April 1998]